OIG in healthcare stands for the Department of Health and Human Services (HHS) Office of Inspector General (OIG) – the Office within the HHS responsible for reducing waste, fraud, and abuse in HHS programs and improving efficiency. The Office is the largest OIG in any Federal Department, and employs more than 1,650 auditors, evaluators, and investigators, who are supported by teams of staff with legal, technological, and analytical experience.
The Background to the Office of Inspector General
The Office of Inspector General for the Department of Health, Education, and Welfare (as the HHS OIG was known as at the time) was created in 1976 to “supervise, coordinate, and provide policy direction for auditing and investigative activities relating to programs and operations of the Department”. The Office was also tasked by Congress to detect and prevent fraud and abuse in programs financed by the Department, and to promote efficiency within the Department.
One of the first tasks undertaken by the newly created OIG in healthcare was to establish the OIG HHS Exclusions List as required by the Medicare-Medicaid Anti-Fraud and Abuse Amendments 1977. However, the task of managing the database of individuals and organizations prohibited from participating in federal health care programs grew substantially following the False Claims Act Amendments of 1986 – overwhelming the Office until the passage of HIPAA in 1996.
Subtitle A of HIPAA Title II created and funded the Health Care Fraud and Abuse Control (HCFAC) program, which gave the OIG in healthcare the resources to enforce §1128 of the Social Security Act – “The Exclusion of Certain Individuals and Entities from Participation in Medicare and State Health Care Programs”. Due to the HCFAC program, the OIG in healthcare now excludes more than 2,000 individuals and organizations per year compared to just thirty-five in 1977/1978.
The Expanding Role of HHS OIG in Healthcare
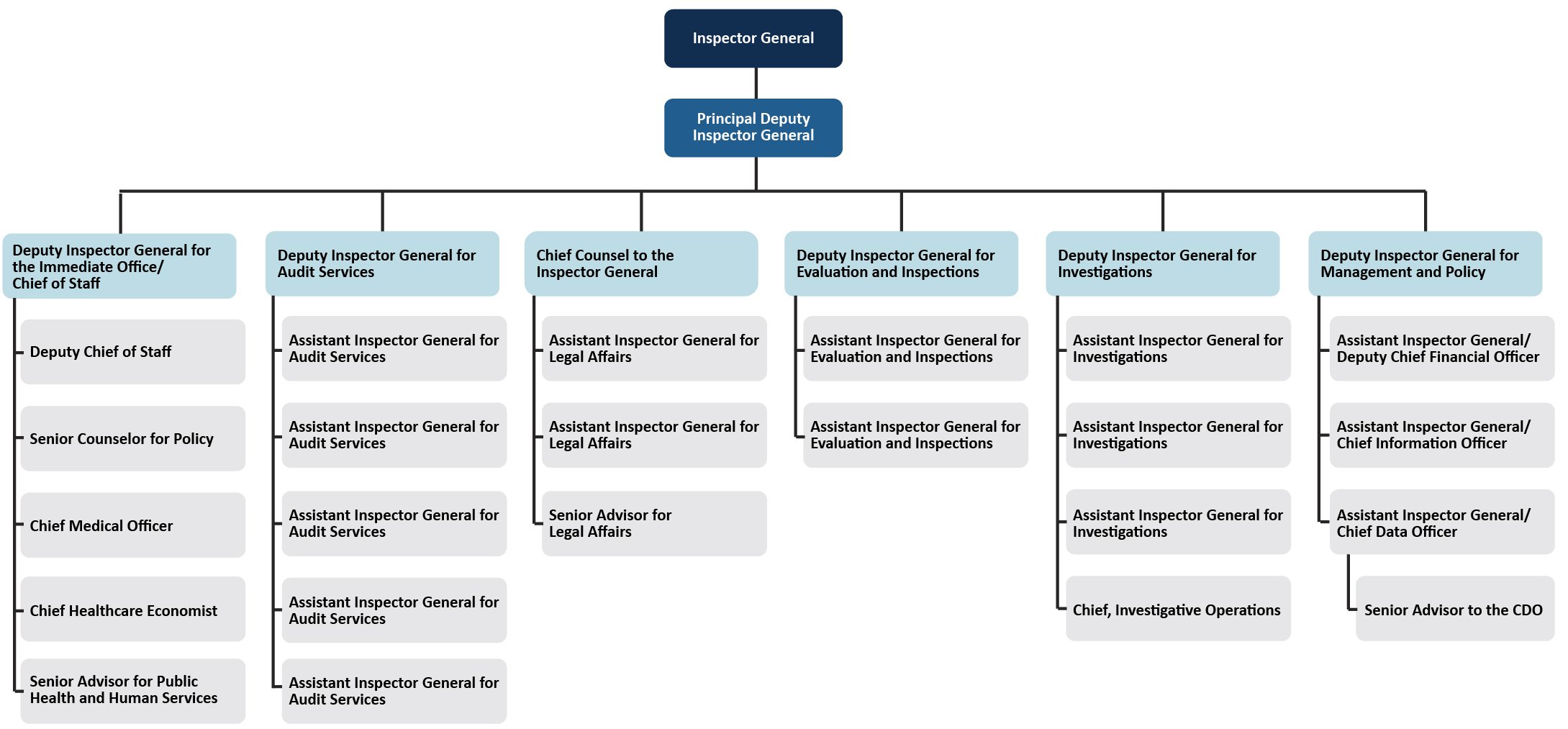
Since its establishment (and the change of name to HHS OIG in 1980), the role of HHS OIG in healthcare has grown significantly. The Office now oversees activities in more than 100 HHS programs, conducts thousands of audits, evaluations, and inspections each year, and provides compliance guidance to tens of thousands of individuals and organizations to encourage compliance with regulations published by HHS agencies such as CMS, CDC, SAMHSA, and OCR. To cope with its expanding role and increasing workloads, HHS OIG divides its work between six sub Offices:
- The Immediate Office of Inspector General, which is directly responsible for the fulfillment of the OIG’s mission.
- The Office of Audit Services, which audits the performance of HHS programs, service providers, and contractors.
- The Office of Counsel to the Inspector General, which acts as an in-house legal counsel to the Inspector General and OIG’s other components.
- The Office of Evaluations and Inspections, which evaluates HHS programs to detect fraud, waste, and abuse and identify opportunities for improvement.
- The Office of Investigations, which conducts criminal, civil, and administrative investigations of fraud and misconduct relating to HHS programs.
- The Office of Management and Policy, which is focused on improving customer satisfaction with, and the reliability of, HHS programs.
Probably the most rapidly expanding role for the HHS OIG in healthcare is cybersecurity. HHS OIG has identified cybersecurity as the top challenge for the healthcare system, and has recently added a Cybersecurity and Information Technology Division to the Office of Audit Services and a Computer Crimes Unit to the Office of Investigations to combat cybersecurity threats within HHS and the healthcare system by fostering enhancements in IT controls, risk management, and resiliency.
Why It Is Important to Understand What the OIG in Healthcare Is
Although the primary role of the OIG in healthcare is to combat fraud, waste, and abuse, and improve the efficiency of HHS programs, the Office also recommends policy changes to agencies within the HHS. When a recommendation is adopted by an HHS agency, it can have a significant impact on the regulations that healthcare providers and their business associates have to comply with. An example of this is the investigation into OCR’s governance of cybersecurity threats.
The OIG investigation is looking into whether the existing Security Rule standards and OCR’s HIPAA audit program are sufficient to prevent and detect cyberattacks, ensure the continuity of patient care, and protect PHI. Although ongoing, the investigation has prompted HHS to publish a Healthcare Sector Cybersecurity Strategy, which not only suggests new HIPAA security standards will be introduced in 2024, but also that compliance with the standards will be a requirement for participation in Medicare.
The post What is OIG in Healthcare? appeared first on HIPAA Journal.
 Patient-centric functionality enhances patient communications with automation, including appointment notification and reminders, online patient scheduling, waitlist management with last-minute cancellation fulfilment, patient experience surveys, and many other features. These can significantly enhance your patients’ perception and experience of your practice.
Patient-centric functionality enhances patient communications with automation, including appointment notification and reminders, online patient scheduling, waitlist management with last-minute cancellation fulfilment, patient experience surveys, and many other features. These can significantly enhance your patients’ perception and experience of your practice. Highlighting the need to p
Highlighting the need to p Reduce No Shows – Up to a 90% improvement in missed appointments.
Reduce No Shows – Up to a 90% improvement in missed appointments. Another
Another  Find out more about the benefits of patient engagement solutions by filling in a form on this page. You will be contacted by a member of staff from Rectangle Health our page sponsor.
Find out more about the benefits of patient engagement solutions by filling in a form on this page. You will be contacted by a member of staff from Rectangle Health our page sponsor. Adding multiple up-to-date payment options leads to improvements in satisfaction and retention levels. For example, making it convenient for patients to pay from their phones by automatically communicating balances and payment options by text and email, practice staff will spend on average 30% less time on payment collection and posting. Plus the practice will see a significant reduction in its accounts receivable numbers.
Adding multiple up-to-date payment options leads to improvements in satisfaction and retention levels. For example, making it convenient for patients to pay from their phones by automatically communicating balances and payment options by text and email, practice staff will spend on average 30% less time on payment collection and posting. Plus the practice will see a significant reduction in its accounts receivable numbers. Contactless patient payment solutions are secure and can protect staff and patients’ health and safety by allowing patients to pay by touching their mobile device or card to a digital reader.
Contactless patient payment solutions are secure and can protect staff and patients’ health and safety by allowing patients to pay by touching their mobile device or card to a digital reader. Multiple financing options are offered to patients just 30 seconds after applying, and the vast majority get approved.
Multiple financing options are offered to patients just 30 seconds after applying, and the vast majority get approved. Part of a modern payment solution suite is a secure online payment gateway, allowing patients to pay online 24 x 7. Optimized for mobile devices, it also works with laptops and desktop computers, allowing patients to make payments from home or on the go.
Part of a modern payment solution suite is a secure online payment gateway, allowing patients to pay online 24 x 7. Optimized for mobile devices, it also works with laptops and desktop computers, allowing patients to make payments from home or on the go. When patients leave a payment method on file, it means one less step during future checkouts. This can even be done ahead of visits when a patient fills out a digital registration form. The front desk can make the payment for the patient at checkout with no need to dig around for cards and a payment receipt will be automatically sent by email.
When patients leave a payment method on file, it means one less step during future checkouts. This can even be done ahead of visits when a patient fills out a digital registration form. The front desk can make the payment for the patient at checkout with no need to dig around for cards and a payment receipt will be automatically sent by email. Card on file also enables healthcare providers to set up an automatically recurring payment to allow a patient to pay down a large out-of-pocket expense over several months. For many patients, having this interest-free option can make the difference between choosing to avail of medical care or not. This flexible payment option is a highly practical way for healthcare providers to receive more incoming payments and for patients to afford their treatment.
Card on file also enables healthcare providers to set up an automatically recurring payment to allow a patient to pay down a large out-of-pocket expense over several months. For many patients, having this interest-free option can make the difference between choosing to avail of medical care or not. This flexible payment option is a highly practical way for healthcare providers to receive more incoming payments and for patients to afford their treatment. Streamlining your payment processes with a patient payment solution that seamlessly integrates with your existing practise management systems brings many business benefits while also providing an improved patient experience.
Streamlining your payment processes with a patient payment solution that seamlessly integrates with your existing practise management systems brings many business benefits while also providing an improved patient experience.